How Bone Density Affects Wisdom Tooth Removal Surgery
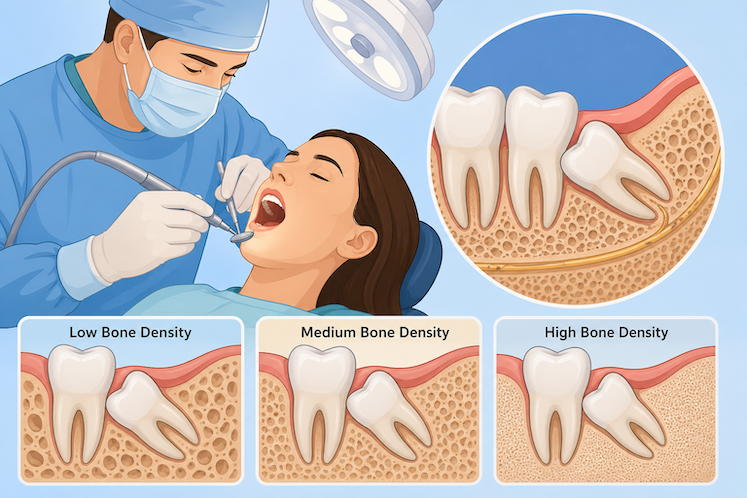
Wisdom tooth removal is not the same for every patient. Some extractions are quick and straightforward, while others require a more careful surgical approach. One of the biggest reasons for that difference is bone density.
Bone density refers to how thick, firm, or compact the jawbone is around the wisdom tooth. When the bone is denser, the tooth may be more firmly anchored, making removal more complex. When the bone is softer or less compact, the tooth may be easier to access and remove.
This is especially important with impacted wisdom teeth, which can grow at an angle, remain trapped under the gums, or stay partially buried in the jawbone. Impacted wisdom teeth may need removal when they cause pain, infection, decay, gum problems, or damage to nearby teeth.
Understanding how bone density affects wisdom tooth removal helps patients feel more prepared, ask better questions, and know what to expect before surgery.
What Bone Density Means in Wisdom Tooth Removal
Bone density is the strength and compactness of the bone surrounding your teeth. In wisdom tooth surgery, it matters because your oral surgeon often needs to work through or around bone to safely remove the tooth.
If a wisdom tooth is fully erupted, bone density may not play a major role. But if the tooth is impacted, tilted, or covered by bone, the density of that bone can affect the surgical plan.
Denser bone can make the tooth harder to loosen. It may also require more sectioning, more precise bone removal, or a longer procedure. Softer bone may allow the tooth to move more easily, but it still requires careful handling to protect the gums, nerves, and surrounding teeth.
Why Wisdom Teeth Are Often Surrounded by Bone
Wisdom teeth, also called third molars, are the last permanent teeth to develop. They typically appear in the late teens or early adult years, when the jaw may not have enough space left for them.
When there is not enough room, the tooth can remain trapped under the gum or jawbone. This is called impaction.
An impacted wisdom tooth may grow sideways, press against the second molar, or sit deep in the jaw. In these cases, the surgeon may need to remove a small amount of bone to reach the tooth safely.
Patients often first notice symptoms such as pressure, jaw discomfort, swelling, or pain near the back molars. These symptoms may overlap with signs that indicate it’s time to schedule an evaluation for third molar extraction.
How Dense Bone Can Make Removal More Complex
Dense jawbone can make wisdom tooth removal more challenging because it holds the tooth more tightly. The surgeon may need to create more space around the tooth before it can be removed.
This does not mean the surgery is unsafe. It simply means the procedure may require more planning, skill, and precision.
During wisdom tooth removal, a dentist or oral surgeon may cut the gum tissue, remove bone blocking access to the root, divide the tooth into sections, clean the site, and place gauze to help a blood clot form.
When bone is very dense, sectioning the tooth into smaller pieces can reduce pressure on the jaw. It also helps the surgeon remove the tooth with less force.
Bone Density and Age: Why Timing Matters
Age can influence bone density around wisdom teeth. Younger patients often have bone that is less dense and more flexible. This can make removal smoother and recovery more predictable.
As patients get older, the jawbone can become denser. Wisdom tooth roots may also become more fully developed, which can make extraction more complicated.
That is one reason many oral surgeons recommend evaluating wisdom teeth during the late teen years or early adulthood. Early evaluation does not always mean immediate removal, but it helps identify whether the teeth are likely to cause future problems.
How Bone Density Affects Surgery Time
Bone density can influence how long wisdom tooth removal takes. A tooth surrounded by softer bone may come out more quickly, especially if it is not deeply impacted.
A tooth surrounded by dense bone may take longer because the surgeon needs to work carefully around the tooth and nearby structures.
More time may be needed for:
- Exposing the impacted tooth
- Removing bone that blocks access
- Separating the tooth into sections
- Protecting nearby nerves and teeth
- Cleaning and closing the surgical area
Even when the procedure takes longer, the goal remains the same: remove the wisdom tooth safely while minimizing trauma to the surrounding tissue.
Bone Density and Anesthesia Planning
Bone density can also affect the overall surgical plan, including anesthesia. A more complex extraction may require a different level of comfort support than a simple removal.
Some patients only need local anesthesia. Others may benefit from sedation, especially if multiple wisdom teeth are being removed or the teeth are deeply impacted.
The type of anesthesia used often depends on the expected difficulty of the removal and the patient’s comfort level. Before surgery, your oral surgeon can explain anesthesia options based on your exam, X-rays, health history, and treatment plan.
How X-Rays Help Evaluate Bone Density
X-rays are one of the most important tools for planning wisdom tooth removal. They show the position of the tooth, the shape of the roots, and how much bone surrounds it.
Imaging also helps the surgeon see whether the wisdom tooth is close to important structures, such as the nerve in the lower jaw or the sinus area in the upper jaw.
While a standard X-ray can provide helpful information, some cases may require 3D imaging. This gives a more detailed view of the tooth and surrounding bone.
The more information your oral surgeon has before the procedure, the more personalized and precise your treatment plan can be.
Dense Bone and Impacted Wisdom Teeth
Impacted wisdom teeth often create the biggest bone-density concerns. If the tooth is fully trapped in the jaw, the surgeon may need to remove bone before the tooth can be accessed.
A deeply impacted lower wisdom tooth can be especially complex because it may sit near the inferior alveolar nerve, which provides sensation to the lower lip, chin, and teeth.
Dense bone around an impacted tooth may require a slower, more controlled approach. Your oral surgeon may remove small amounts of bone, section the tooth, and carefully elevate each piece.
This technique helps reduce unnecessary pressure on the jaw.
Does Low Bone Density Make Removal Easier?
In some cases, lower bone density may make it easier to loosen and remove a wisdom tooth. However, softer bone does not automatically mean the procedure is simple.
Other factors still matter, including:
- Tooth angle
- Root shape
- Depth of impaction
- Gum inflammation
- Infection
- Proximity to nerves or sinuses
- Number of wisdom teeth being removed
A tooth with curved roots or a difficult angle can still require a surgical approach, even if the surrounding bone is not especially dense.
Bone Density and Recovery After Wisdom Tooth Removal
Bone density may also influence recovery. If more bone needs to be removed during surgery, there may be more swelling, soreness, or jaw stiffness afterward.
Some pain, bleeding, swelling, and temporary difficulty opening the mouth can happen after wisdom tooth extraction. These symptoms are usually manageable with proper aftercare and medication instructions.
Healing happens in stages. The gum tissue may start feeling better within days, but deeper tissue and bone take longer to recover. If you want to understand the full healing process, learning how gums fully heal can help you set realistic expectations after surgery.
The Role of the Blood Clot in Bone Healing
After a wisdom tooth is removed, a blood clot forms in the socket. This clot protects the bone and nerves underneath while healing begins.
If the clot becomes dislodged or fails to form properly, dry socket can occur. Dry socket exposes the bone and nerves, causing significant pain that often begins one to three days after extraction.
This is why post-operative instructions matter. Avoiding straws, smoking, vigorous rinsing, and hard foods during early healing can help protect the clot.
Eating After Surgery When Bone Removal Was Needed
If your wisdom tooth removal involved dense bone or a deeper impaction, your mouth may be more tender during the first few days. Soft foods can make recovery easier.
Good early options may include yogurt, applesauce, smoothies without a straw, mashed potatoes, soup that is not too hot, scrambled eggs, and soft pasta.
Avoid crunchy, spicy, sticky, or hard foods until your surgeon says it is safe. These foods can irritate the socket or disturb the healing clot.
For a more structured recovery routine, a surgery meal plan can make the first week feel less stressful.
How Surgeons Reduce Trauma During Removal
Experienced oral surgeons use several techniques to make wisdom tooth removal safer and more comfortable, especially when bone density is a factor.
One common method is tooth sectioning. Instead of pulling the entire tooth out at once, the surgeon divides it into smaller parts. This reduces the amount of force needed.
Another technique is conservative bone removal. The surgeon removes only the bone necessary to access the tooth safely.
The goal is not just to remove the tooth. It is to protect the surrounding bone, gums, nerves, and nearby teeth while helping the patient recover as smoothly as possible.
When Bone Density May Increase Surgical Risk
Bone density alone does not usually make wisdom tooth surgery risky. However, it can add complexity when combined with other factors.
Risk may increase when:
- The tooth is deeply impacted
- Roots are close to a nerve
- The patient is older
- The tooth has curved or long roots
- There is infection or inflammation
- Multiple teeth are being removed
- The surrounding bone is very compact
This is why a consultation is so important. Your surgeon can review your imaging, explain the level of difficulty, and recommend the safest approach.
Why Personalized Treatment Matters
No two wisdom tooth cases are exactly alike. One patient may have four wisdom teeth that are simple to remove. Another may have one impacted tooth surrounded by dense bone that needs a more advanced surgical plan.
Personalized care helps your oral surgeon decide:
- Whether removal is necessary
- When removal should happen
- What anesthesia is appropriate
- How complex the surgery may be
- What recovery instructions you need
- Whether special imaging is recommended
If you are dealing with wisdom tooth pain, pressure, or swelling, it is better to get evaluated early rather than wait for symptoms to worsen. Get a professional opinion based on your specific tooth position and jaw structure.
What Patients Can Do Before Surgery
You cannot change your bone density before wisdom tooth removal, but you can prepare well.
Before surgery, tell your oral surgeon about any medications, health conditions, smoking habits, or previous dental issues. This helps the team plan your care safely.
You should also follow instructions about eating, drinking, transportation, and medication use before the procedure.
Good preparation can make the surgery day smoother and reduce stress.
What Patients Can Do After Surgery
After surgery, follow your post-op instructions closely. This is especially important if your extraction involved dense bone, deep impaction, or multiple wisdom teeth.
Helpful recovery steps include:
- Resting for the first day
- Using gauze as instructed
- Applying cold packs if recommended
- Eating soft foods
- Avoiding straws
- Avoiding smoking or vaping
- Keeping the mouth clean without aggressive rinsing
- Taking medications as directed
If pain suddenly gets worse after initially improving, contact your oral surgeon. Increasing pain, foul odor, bad taste, or visible bone may be signs of dry socket.
FAQ About Bone Density and Wisdom Tooth Removal
Does dense bone make wisdom tooth removal painful?
Dense bone can make the procedure more complex, but it should not make the surgery painful during treatment. Your mouth will be numbed, and sedation may be available depending on your case.
You may feel more soreness afterward if the tooth was deeply impacted or required more bone removal.
Can X-rays show bone density around wisdom teeth?
X-rays can show how much bone surrounds the tooth and how the tooth is positioned. In more complex cases, 3D imaging may be used for a clearer view.
This helps the surgeon plan the safest approach.
Is wisdom tooth removal harder for adults?
It can be. Adult jawbone may be denser, and wisdom tooth roots may be more developed. This can make removal more complex than it often is for younger patients.
However, many adults still have successful wisdom tooth removal with proper planning.
Does bone grow back after wisdom tooth removal?
The socket gradually fills in as healing progresses. Gum tissue heals first, while deeper bone remodeling takes longer.
Your oral surgeon can explain what healing should look like based on your procedure.
Can dense bone cause dry socket?
Dense bone itself is not the only cause of dry socket. Dry socket happens when the protective blood clot is lost, fails to form, or dissolves too early. Difficult extractions and surgical site trauma may contribute to risk.
Following aftercare instructions is one of the best ways to reduce that risk.
Should all impacted wisdom teeth be removed?
Not always. Some impacted wisdom teeth are monitored if they are not causing problems. Others need removal because they cause pain, infection, decay, gum disease, cysts, or damage to nearby teeth.
A consultation and imaging are the best way to know what is right for your case.
Conclusion
Bone density plays an important role in wisdom tooth removal. Dense bone can make surgery more complex, while softer bone may allow for easier tooth movement. Still, bone density is only one part of the picture.
Tooth position, root shape, impaction depth, age, symptoms, and nearby nerves all affect the treatment plan.
The good news is that experienced oral surgeons evaluate these details before surgery. With proper imaging, anesthesia planning, and aftercare, wisdom tooth removal can be handled safely and comfortably.
Wisdom Teeth vs. Other Molars: What’s the Real Difference?
January 1, 2026

Wisdom Tooth Surgery Mistakes That Slow Your Healing
April 28, 2026

What Counts as a Dental Emergency?
January 14, 2026

What to Bring to Your Oral Surgery Appointment: Essential Checklist
December 29, 2025

When Should Wisdom Teeth Be Removed? Warning Signs to Know
May 15, 2026