Wisdom Tooth Nerve Damage: How Rare Is It, Really?
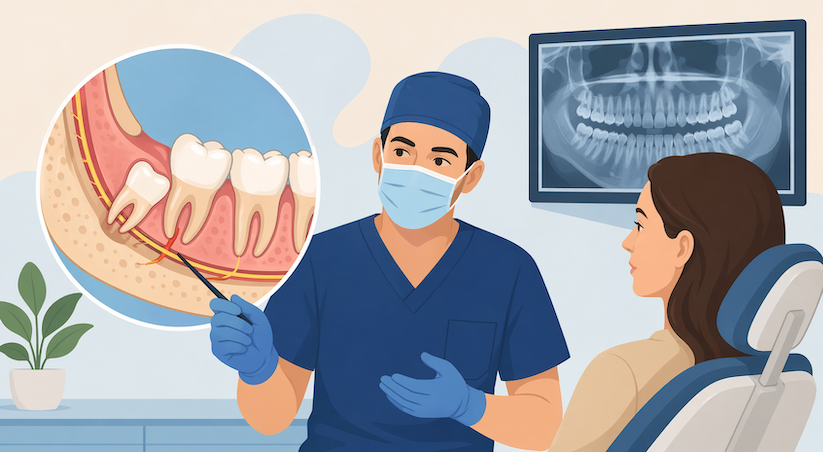
Hearing the words “nerve damage” before wisdom tooth removal can make even a routine procedure sound alarming. It is one of the most searched concerns around extraction, and for good reason. When a lower wisdom tooth sits close to a major nerve, patients naturally want to know what the real risk is, how often it happens, and what can be done to reduce it.
The reassuring truth is that nerve damage from wisdom tooth removal is uncommon, and permanent nerve injury is rarer still. Most wisdom tooth extractions heal without any lasting issue. Even in cases where there is temporary numbness, many patients recover gradually over weeks or months. The key is proper evaluation, careful surgical planning, and choosing an experienced provider who understands how to manage higher-risk cases.
In this article, we will break down what nerve damage actually means, why it can happen, how rare it is, what symptoms to watch for, and how surgeons work to protect the nerves during wisdom tooth removal. If you have been told your tooth is close to a nerve, this guide will help you understand the risk in a calm, practical way.
What Nerve Damage Means After Wisdom Tooth Removal
When people talk about nerve damage after wisdom tooth extraction, they are usually referring to irritation or injury involving one of two nerves in the lower jaw.
The first is the inferior alveolar nerve. This nerve runs inside the lower jawbone and provides feeling to the lower lip, chin, and lower teeth on one side. The second is the lingual nerve, which affects sensation in the tongue and nearby tissues.
If one of these nerves becomes bruised, stretched, compressed, or irritated during extraction, a patient may notice numbness, tingling, altered sensation, or a pins-and-needles feeling. In most cases, this is temporary. The nerve is not necessarily severed or permanently harmed. It may simply be inflamed from the procedure or from the position of the tooth.
That distinction matters. Temporary nerve symptoms are very different from permanent nerve damage, and the two should not be treated as if they are equally likely.
Why Wisdom Teeth Can Be Close to Important Nerves
Lower wisdom teeth develop in a part of the jaw where space is limited. In some patients, the roots form very close to the inferior alveolar nerve canal. In others, the angle of the tooth or its impaction pattern can make removal more complex.
This is one reason early evaluation matters. A tooth that is partially trapped under the gum or bone can shift, press against neighboring teeth, or develop roots that are harder to remove later. When surgeons review imaging ahead of time, they look carefully at the relationship between the tooth roots and surrounding nerve structures.
If you are still deciding where to go, choosing the right extraction clinic can make a meaningful difference in how thoroughly your case is assessed before surgery.
How Rare Is Nerve Damage, Really?
This is the question most patients care about most, and the answer is generally reassuring.
Nerve injury after wisdom tooth removal is rare overall. Temporary nerve disturbances do happen in a small percentage of cases, especially when lower wisdom teeth are deeply impacted or very close to a nerve. Permanent nerve damage is much less common.
The exact percentage varies depending on the position of the tooth, the anatomy of the patient, the imaging used, and the difficulty of the extraction. Higher-risk cases tend to involve lower wisdom teeth that sit deep in the jaw or have roots that appear to overlap the nerve canal on X-rays.
Still, most extractions do not result in nerve problems. And among the patients who do notice numbness or altered sensation afterward, many improve with time as the nerve recovers.
So if you are wondering whether nerve damage is possible, the honest answer is yes. If you are wondering whether it is common, the answer is no. If you are worried it is usually permanent, that is also no.
Which Wisdom Teeth Carry the Highest Risk?
Not all wisdom teeth pose the same level of concern.
Lower Wisdom Teeth
The risk discussion is mostly about lower wisdom teeth, especially impacted ones. That is because the inferior alveolar nerve travels through the lower jaw, close to where the roots of the lower third molars may form.
Deep Impactions
A deeply impacted tooth buried in bone may require more surgical manipulation than a tooth that has already erupted. More complex removal can increase the chance of temporary nerve irritation.
Roots Near the Nerve Canal
If imaging shows the tooth roots appear very close to the nerve canal, your surgeon may discuss a slightly higher chance of numbness after surgery. That does not mean nerve damage will happen. It means your case needs careful planning.
Unusual Anatomy
Every patient is different. Root shape, bone density, age, and the exact path of nearby nerves can all influence the difficulty of the procedure.
Symptoms That May Suggest Nerve Irritation
After wisdom tooth removal, some normal numbness is expected at first because local anesthesia is still wearing off. That is not nerve damage. The question is what symptoms remain after the anesthetic should have fully faded.
Potential nerve-related symptoms may include:
Numbness in the Lip or Chin
This can happen if the inferior alveolar nerve is affected. The area may feel partially numb, tingly, or less responsive than usual.
Tingling or Altered Sensation
Some patients describe it as pins and needles, a crawling feeling, or unusual sensitivity.
Tongue Numbness or Taste Changes
If the lingual nerve is irritated, the tongue may feel numb or strange on one side. Some people notice mild taste changes as well.
Persistent Sensation Changes Beyond the Expected Recovery Window
If numbness continues after the initial post-operative period, it should be reported to your surgeon so it can be monitored properly.
It is also worth remembering that jaw discomfort can come from several different causes. In some cases, patients confuse nerve concerns with bite-related pain or inflammation. If you have dealt with pain when biting before, you may already know how different dental symptoms can overlap.
Temporary vs Permanent Nerve Damage
This is one of the most important parts of the conversation.
Temporary Nerve Symptoms
Temporary symptoms are more common than permanent injury. The nerve may be irritated during surgery, especially if the tooth sits very close to it. This can lead to numbness, tingling, or altered sensation for a period of time.
Recovery may happen over days, weeks, or months depending on the degree of irritation. Many patients improve steadily as healing progresses.
Permanent Nerve Injury
Permanent nerve damage is rare. It usually refers to symptoms that do not fully resolve over time. While this is the risk patients fear most, it is not the typical outcome.
The fact that your surgeon discusses this possibility does not mean it is likely. It means informed consent is being taken seriously and your care team wants you to understand the full picture.
How Surgeons Reduce the Risk
Good surgical planning is the biggest reason wisdom tooth removal is generally safe.
Detailed Imaging
A standard panoramic X-ray often gives a clear first look at the position of the wisdom tooth and nearby nerve canal. In cases that appear more complex, a 3D scan may be recommended to better understand the anatomy.
This extra information helps the surgeon plan the safest way to remove the tooth.
Surgical Technique
An experienced oral surgeon uses techniques designed to minimize pressure on surrounding structures. That includes how the gum is opened, how bone is removed if needed, and whether the tooth is sectioned into smaller pieces for gentler removal.
Case Selection
Some patients benefit from earlier removal before roots fully develop or before the tooth becomes more difficult to access. In other cases, the surgeon may adjust the treatment plan based on the level of risk.
Clear Follow-Up
If unusual numbness occurs, prompt follow-up allows the surgeon to track recovery and recommend next steps. Monitoring matters, and patients should never feel they need to guess whether a sensation change is normal.
When a Coronectomy May Be Considered
In selected high-risk cases, a coronectomy may be discussed. This is a procedure where the crown of the wisdom tooth is removed but the roots are intentionally left in place because they are too close to the nerve.
This option is not right for everyone, but it can be useful when the goal is to reduce the chance of nerve injury while still addressing the problematic part of the tooth.
A surgeon will only recommend this when it makes sense for the anatomy and the overall condition of the tooth.
Factors That Can Affect Your Individual Risk
General statistics are helpful, but your risk depends on your specific situation.
Age
Wisdom tooth removal is often simpler in younger patients because roots may be less developed and bone may be less dense. As patients get older, extractions can sometimes become more technically demanding.
Tooth Position
A partially erupted tooth is different from a fully impacted one. A tilted, sideways, or deeply buried tooth may be more complex to remove.
Root Formation
Long, curved, or fused roots can add complexity, especially if they track near the nerve canal.
Existing Symptoms or Infection
Inflammation, infection, cysts, or repeated gum problems around the wisdom tooth can influence both timing and treatment recommendations.
Surgical Experience
The training and judgment of the provider matter. Careful planning, precise technique, and strong case evaluation all help reduce avoidable risk.
What Recovery Usually Feels Like
Most patients recover from wisdom tooth removal with swelling, soreness, and mild limitation in jaw opening for a few days. These are normal healing responses and not signs of nerve damage.
You may also notice temporary numbness from anesthesia immediately after the procedure. That should gradually wear off. What you want to pay attention to is any lingering numbness that feels unusual hours later or the next day.
Good recovery also depends on following post-op instructions closely. Eating soft foods, keeping the area clean, avoiding smoking, and protecting the blood clot all help support healing.
Some patients underestimate how much tension affects the body during recovery. Increased clenching and jaw tightness can make discomfort feel worse, which is one reason understanding stress and jaw issues can be helpful when healing feels more intense than expected.
When You Should Call the Surgeon
You should contact your surgeon if you notice:
- Numbness in the lip, chin, or tongue that does not improve after the anesthetic should have worn off
- Tingling or altered sensation that seems unusual or persistent
- Difficulty speaking, eating, or controlling the tongue normally
- Severe or worsening pain that feels out of proportion to normal recovery
- Signs of infection such as fever, pus, or swelling that keeps getting worse
Do not wait and hope something important will sort itself out. Most post-op questions turn out to be manageable, but checking in early is always the smarter move.
How Nerve Symptoms Are Managed If They Happen
If nerve symptoms do occur, your surgeon will usually begin with careful monitoring. The first step is documenting exactly what you feel, where the numbness is located, and whether it changes over time.
Follow-up visits may include sensory testing and regular progress checks. Some cases improve steadily without further treatment. If symptoms are more significant or prolonged, your surgeon may discuss additional evaluation or referral.
What matters most is early communication and realistic expectations. Recovery is often gradual rather than instant.
Should Fear of Nerve Damage Stop You From Removing Wisdom Teeth?
For most people, no.
It is reasonable to ask thoughtful questions and want a clear explanation before surgery. That is what good consultation is for. But in many cases, avoiding necessary removal can create a different set of problems, including infection, gum inflammation, damage to nearby teeth, crowding concerns, or recurring pain.
Leaving a problematic wisdom tooth in place is not automatically the safer choice. The better question is whether the benefits of removal outweigh the risks in your specific case.
That decision should be based on your imaging, symptoms, age, and clinical exam, not just on a worst-case scenario you found online.
How to Feel More Confident Before Surgery
If you are anxious about nerve damage, a few simple steps can help you feel more prepared.
Ask for a Clear Review of Your Imaging
Have the provider explain where the tooth sits, whether it appears close to a nerve, and what that means in practical terms.
Ask About Your Personal Risk, Not Just General Risk
Two patients with wisdom teeth are not automatically facing the same situation. Your anatomy matters.
Understand the Plan
Ask how the tooth will be removed, whether any special imaging is needed, and what the follow-up process looks like if numbness occurs.
Prepare for Recovery
Having a solid recovery plan can reduce anxiety. Stock up on soft foods, arrange transportation, and follow your aftercare instructions carefully.
Even small comfort steps matter after surgery. Patients often focus only on pain and swelling, but everyday habits like hydration and fresh breath habits can also make recovery feel cleaner and easier.
The Bottom Line on Nerve Damage Risk
Nerve damage from wisdom tooth removal is possible, but it is rare, and permanent injury is rarer still. The majority of patients recover without lasting nerve problems. Temporary numbness can happen in a small number of cases, particularly when lower wisdom teeth are very close to the nerve, but even then, many patients improve over time.
The best way to reduce risk is to have the tooth evaluated properly, understand your anatomy, and work with a qualified provider who takes imaging and surgical planning seriously. Fear is understandable, but it should be balanced with facts.
If your wisdom teeth are causing pain, swelling, repeated infections, or concern on imaging, the next step is not panic. It is getting a professional opinion and understanding your options. When you are ready to schedule your consultation, a personalized exam can tell you far more than general statistics ever will.

Wisdom Tooth Extraction: Dentist vs. Oral Surgeon
January 30, 2026

How Long Does Wisdom Tooth Surgery Really Take?
February 20, 2026

How to Sleep After Wisdom Tooth Surgery Fast
February 25, 2026

Sleep Dentistry for Wisdom Tooth Removal: Is It Right?
April 3, 2026

Is It Safe to Fly After Wisdom Tooth Removal?
March 12, 2026